Weekly Checkup
April 13, 2018
Addressing the Opioid Crisis
In the United States, opioids are now involved in more than 42,000 deaths annually, and last year overdoses became the number one cause of death for Americans under the age of 50. Further, the Centers for Disease Control and Prevention has pegged the costs of the epidemic at $78.5 billion.
While the opioid crisis has been building for over a decade, in many ways the country and policymakers are still coming to terms with the full scope of the challenge. Congress was busy at work on the issue this week, with the House Ways and Means Committee releasing a white paper of recommendations, the Senate Health, Education, Labor and Pensions Committee gearing up for a markup later this month on the bipartisan Opioid Crisis Response Act of 2018, and the House Energy and Commerce Committee holding a hearing on the role the Medicare and Medicaid programs can play in combatting the opioid crisis.
Over the last few months, AAF experts Ben Gitis and Tara Hayes—along with some of our fantastic interns (apply here)—have been digging into the opioid crisis through a series of studies. Hayes provides an a excellent primer on the current state of the opioid crisis, the origins of the crisis, and the policy debate around addressing the crisis at present (read it here). Gitis has written about both the crisis’ impact on the labor market (helpfully summarized in this video and this infographic), as well as the failure of prescribing reforms to stem the overall increase in opioid-related deaths. All three pieces are worth your time, and collectively they paint a clearer picture of where the epidemic stands today.
A few points are worth noting. First, while efforts to reform prescribing practices and the formulation of prescription pain medication have had an effect, the rate of opioid-related deaths is accelerating as illicit, non-prescription opioids such as heroin and more potent synthetic alternatives have flooded the market to meet demand.
Second, the economic implications of the crisis have been under appreciated. AAF found that roughly one million prime-age workers have been lost to the workforce as a result of the crisis, causing a 0.2 percentage point reduction in annual economic growth.
Third, while an overabundance of opioids has contributed to the growing epidemic, any long-term solution will have to focus on substance abuse and mental-health treatment. Reducing the supply of prescription opioids has meant that those suffering from substance abuse disorders have simply shifted to alternative drugs. Economic factors (such as unemployment) may play a role in driving some people to opioid abuse; however, breaking the cycle of addiction requires proven treatment methods.
Chart Review
Tara O’Neill Hayes, Deputy Director of Health Care Policy
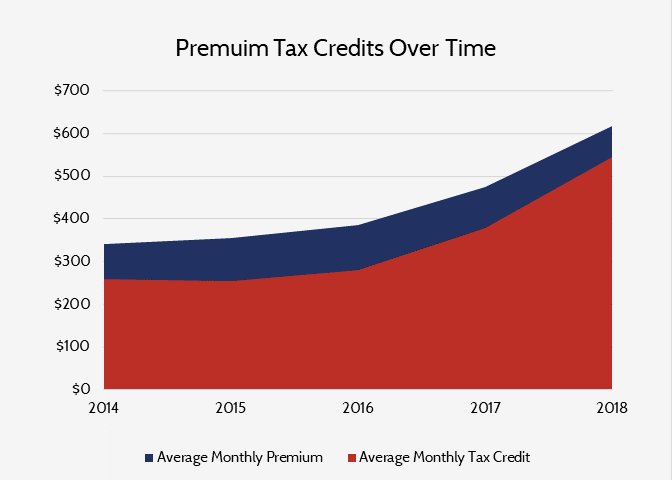
Premiums in the individual market have increased substantially each year since the passage of the Affordable Care Act, but despite the market finally beginning to stabilize, this year saw the largest increase in premiums to date. These increases were primarily a result of the Trump Administration’s decision no longer to pay the cost-sharing reduction subsidies following a court decision that their payment was unconstitutional. Not paying those subsidies, however, has dramatically increased the cost of premium subsidies, as shown in the chart below and explained here.
Worth a Look
Axios: The left is getting more active on health care
Wall Street Journal: NEA Backs Startup’s Software to Assess Drug Performance