Research
September 10, 2020
Chronic Disease in the United States: A Worsening Health and Economic Crisis
Executive Summary
- The prevalence and cost of chronic disease in the United States is growing and will continue to grow, not just as a result of the Baby Boomer generation aging but also due to increased disease prevalence among children and younger adults.
- The prevalence of chronic disease varies greatly across the country with a higher concentration in the Mid-South region.
- Those with chronic disease and their families face both direct and indirect costs: Direct costs primarily stem from longer and more frequent hospital visits and greater prescription drug use, while indirect costs arise from lost education and job opportunities.
- When including indirect costs associated with lost economic productivity, the total cost of chronic disease in the United States reaches $3.7 trillion each year, approximately 19.6 percent of the country’s gross domestic product.
Introduction
Chronic disease in the United States, already highly prevalent, is expected to worsen over the next several decades among all age groups. The burden of the associated physical and economic costs will worsen, as well. But the burdens of chronic disease do not just loom in the future: Evidence suggests that the high prevalence of chronic disease may be partially responsible for the devastating effects of the current coronavirus pandemic.[1] Further, the economic consequences of the pandemic have made it even more difficult for the United States to afford the growing health care costs that result from chronic disease.
A disease is considered chronic when it persists for at least a year and requires ongoing medical attention or limits daily activities.[2] Approximately 47 percent of the U.S. population, 150 million Americans, suffered from at least one chronic disease, as of 2014.[3] Almost 30 million Americans are living with five or more chronic diseases.[4] The risk and prevalence of chronic disease grows as individuals age. Approximately 27 percent of children in the United States suffer from a chronic condition, while about 6 percent of children have more than one chronic condition.[5] In contrast, around 60 percent of adults suffer from at least one chronic condition, while 42 percent suffer from multiple conditions.[6] Among those 60 or older, at least 80 percent have one chronic illness and 50 percent have two.[7] These ailments account for 70 percent of all deaths in America, killing more than 1.7 million people each year.[8]
The share of health care costs borne by those with chronic disease are disproportionate to the number of people affected. An estimated 84 percent of health care costs are attributed to the treatment of chronic disease.[9] The rates are even higher for beneficiaries in public health insurance programs: 99 percent of Medicare and 80 percent of Medicaid spending went toward the treatment of chronic diseases, as of 2010.[10] Given the correlation between chronic disease and age, this health and cost burden is only expected to grow: It’s estimated that by 2060, the U.S. population aged 65 years and older will more than double, from 46 million today to 98 million.[11]
Change in Prevalence Over Time
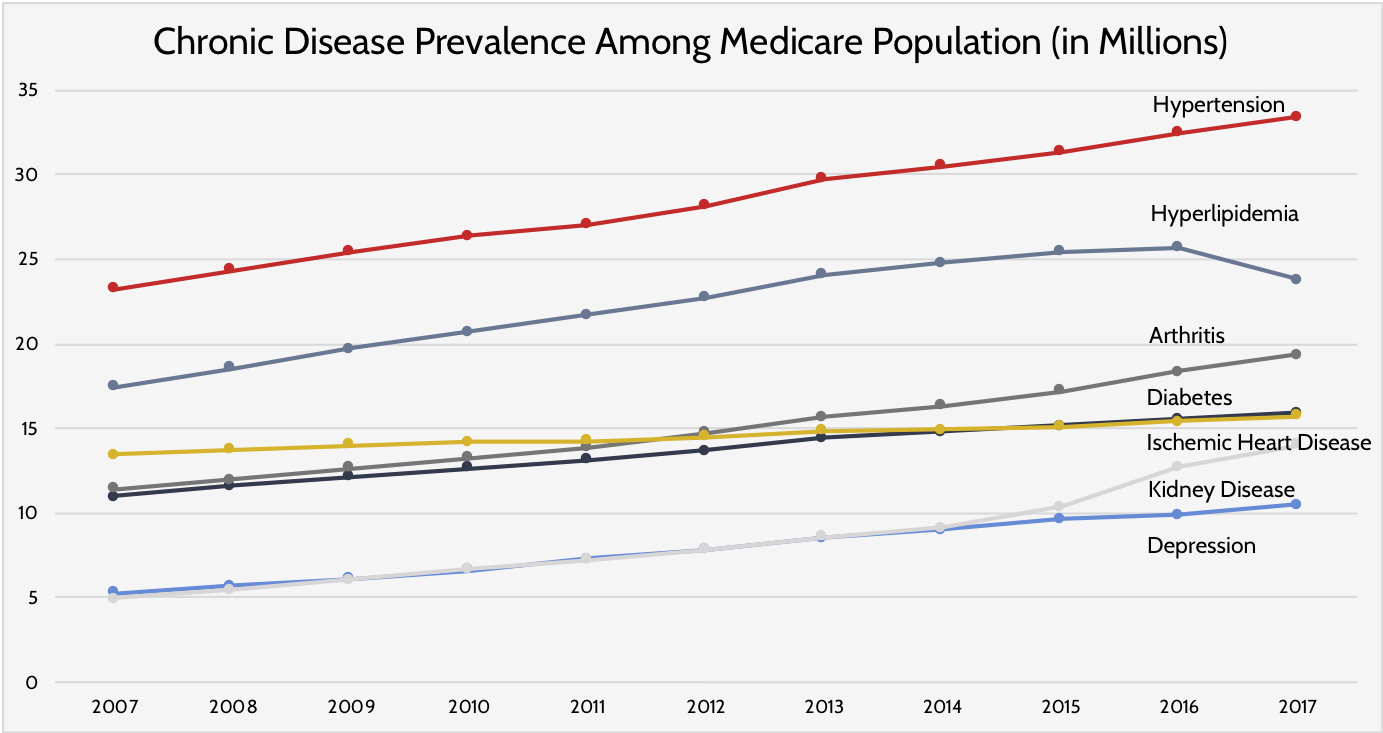
The growth in the number of individuals with chronic diseases is likely to continue at the same trajectory as existing trends shown. As shown in Figure 1, the number of Medicare beneficiaries suffering from any of the diseases defined as “chronic” by the Centers for Medicare and Medicaid Services (CMS), other than hyperlipidemia (resulting from high levels of fat particles (lipids) in the blood), has grown steadily from 2007 to 2017.[12]
Figure 1:
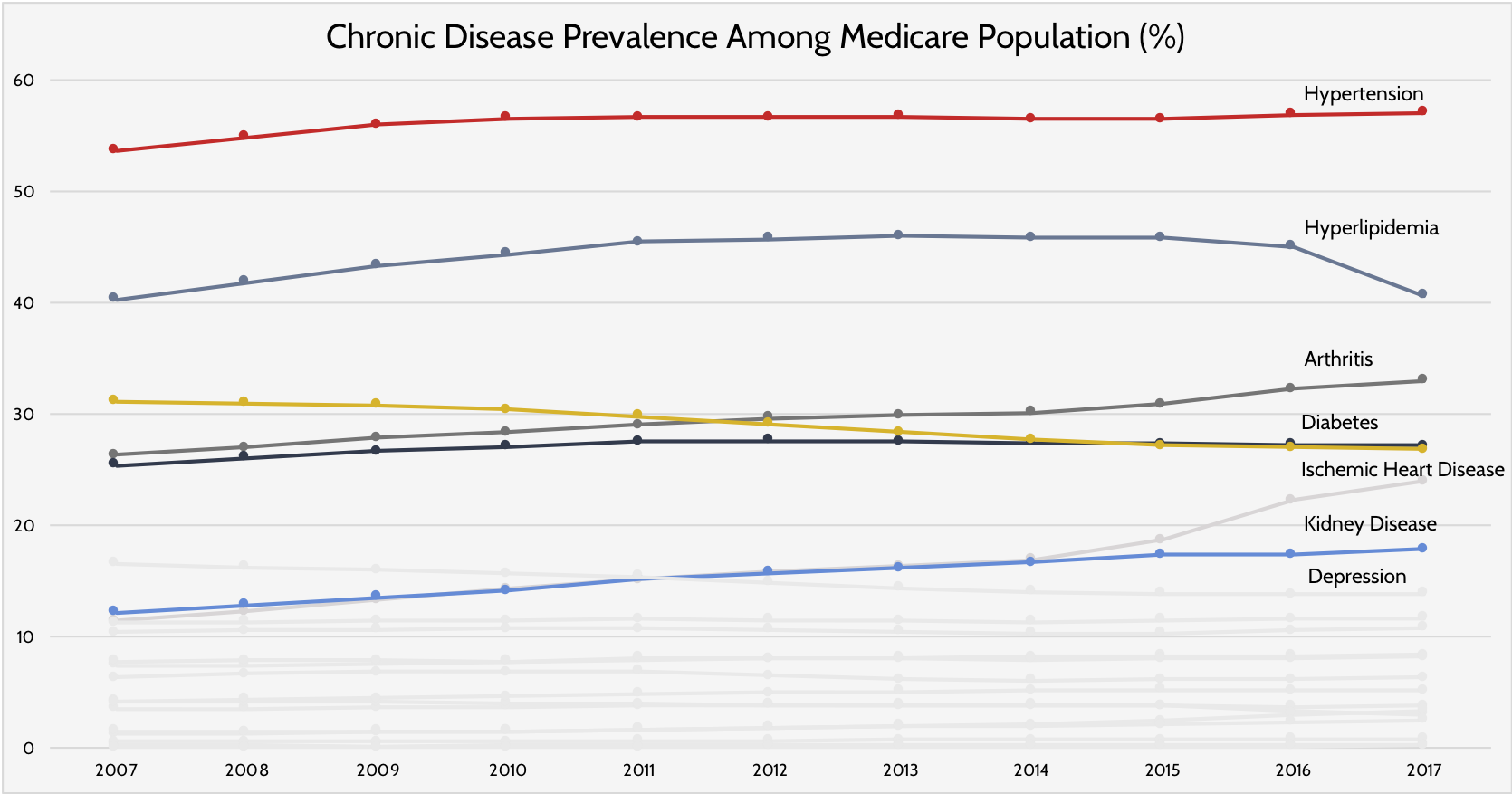
It does not appear, however, that this growth is driven by a heightened prevalence of chronic disease but rather a growth in the population that is most affected by it. This distinction can be seen in Figure 2. With the exception of kidney disease, arthritis, and depression, the proportion of the Medicare population suffering from chronic disease has not grown significantly, while the prevalence of some diseases has even decreased.[13] These trends imply that the risk of chronic disease is not growing among this population.
Figure 2:
While the risk of chronic disease is not growing among older adults, the incidence among older adults is, and this growth is not just occurring in this demographic. A recent study comparing the prevalence of 17 chronic diseases among various age groups between 2005 and 2014 found increases in nearly every disease, including in the youngest groups in the study: 35-50 years old and 51-65 years old.[14] Children have similarly suffered from increasing rates of chronic disease. Less than 2 percent of children in 1960 had a health condition severe enough to interfere with activities of daily life; 50 years later, more than 8 percent of children had such a condition.[15] Much of the increase is associated with greater prevalence of four types of conditions: asthma, obesity, mental health conditions, and neurodevelopmental disorders (which affect brain developmental and may result in neuropsychiatric problems or impaired motor function, learning, or communication skills).[16] In the last three decades, the prevalence of obesity has more than doubled in children and tripled in adolescents, reaching nearly 19 percent overall as of 2016.[17] Between 2001 and 2009, the prevalence of juvenile diabetes increased 23 percent.[18] In 2012, University of Michigan estimated that between 15 to 18 percent of children had at least one chronic condition.[19]
Geographic Variation
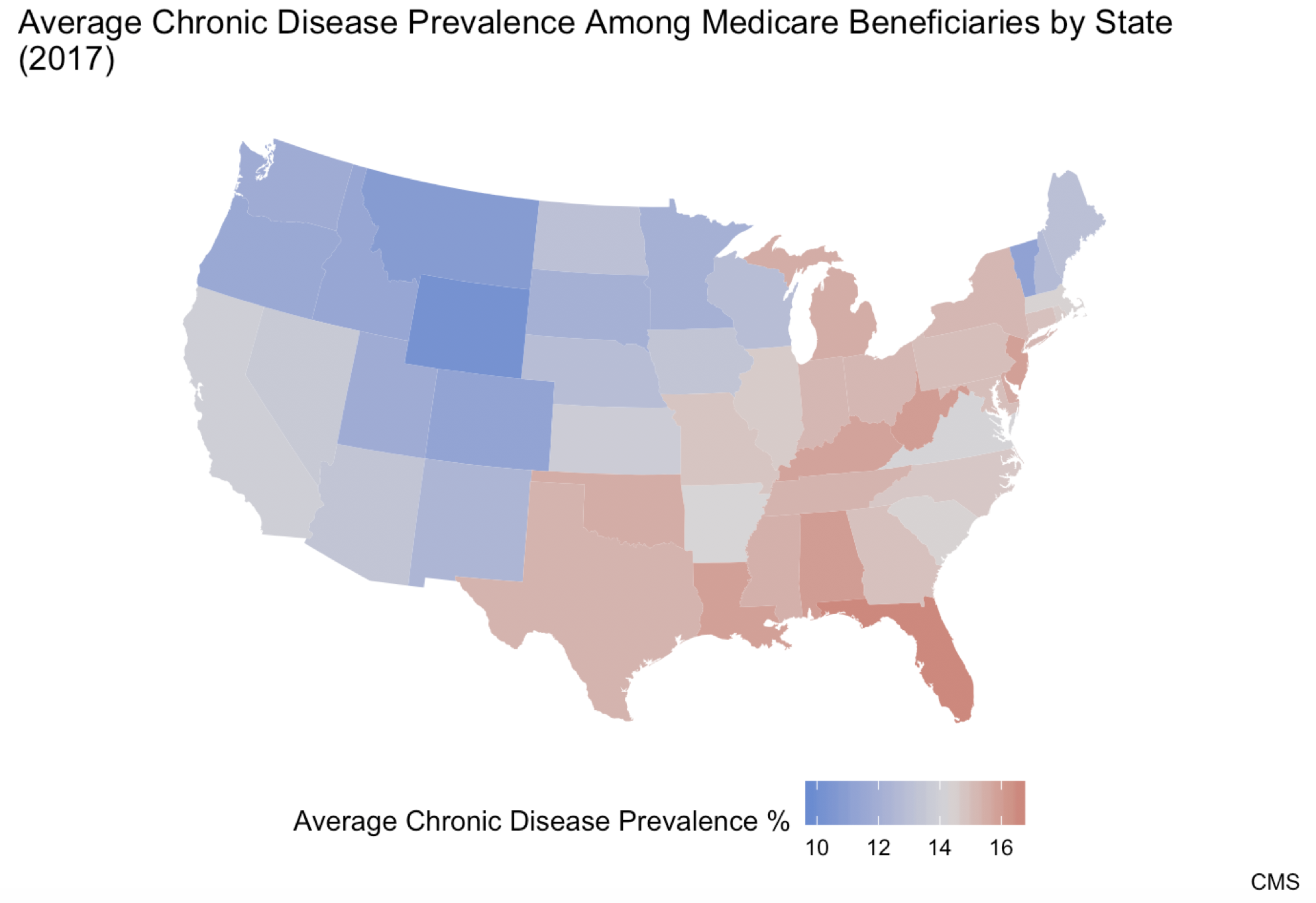
Although chronic disease affects approximately half of the U.S. population, there are parts of the country facing a far higher burden than others. Figure 3 displays the distribution of chronic disease among Medicare beneficiaries in the United States. Each state has been given its own average chronic disease prevalence value, calculated by summing the proportions of Medicare beneficiaries suffering from each of 21 different chronic diseases in a state and dividing the sum by 21, the total number of chronic diseases measured.[20]
Figure 3:
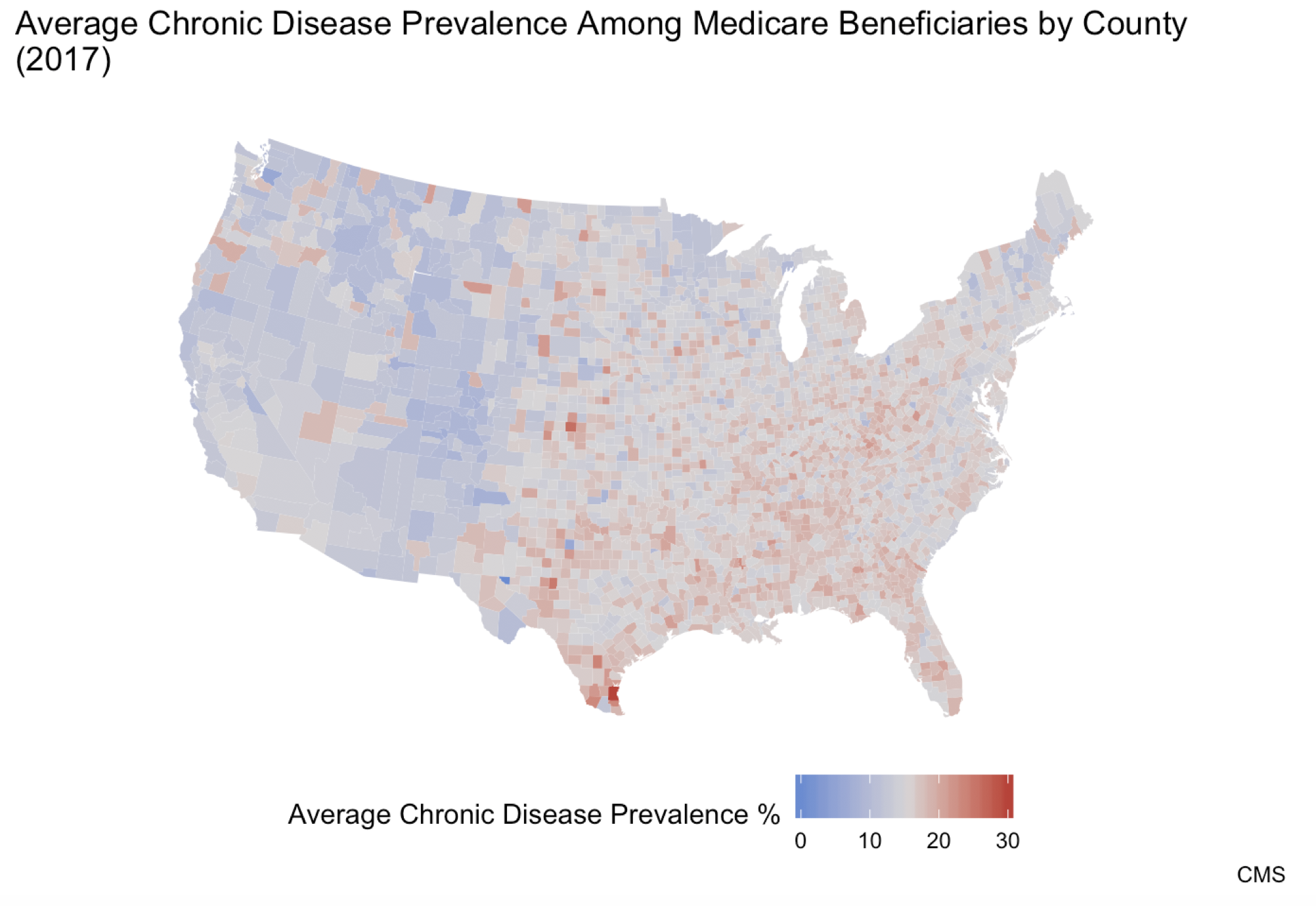
As seen above, the highest prevalence of chronic disease is concentrated in the Mid-South region. The state with the highest average chronic disease prevalence—16.6 percent—is Florida. The state with the lowest average chronic disease prevalence is Wyoming at 9.8 percent. Note that because these prevalence rates are based on the percentage of the Medicare population with a given disease within each state, Florida’s prevalence rate is not higher simply because it is home to a larger share of Medicare beneficiaries than other states. It’s also important to note that within the states, there is even further variation at the county level, as shown in Figure 4. The county with the highest average chronic disease prevalence is Kenedy County, Texas with a disease prevalence of 30.0 percent. Multiple counties share the status of lowest prevalence with an average chronic disease prevalence of 0.0 percent, including Loving County, Texas. This goes to show the degree of variation that can exist within a single state.
Figure 4:
Mechanisms driving this geographic variation include social determinants such as income, education, and health care access, as well as the racial makeup of a given area. In states and counties with higher proportions of minorities, chronic disease is often more prevalent, driven by a multitude of factors.
Costs
The costs associated with chronic disease in the United States, both direct and indirect, are immense. Direct costs are those attributed to the prescriptions, procedures, and other health care products and services needed to treat individuals with chronic diseases. Indirect costs are those associated with the impacts of chronic disease in other realms of life, such as effects on employment, mobility, and other factors associated with well-being. When including indirect costs associated with lost economic productivity, the total cost of chronic disease in the United States reaches $3.7 trillion each year, approximately 19.6 percent of the country’s gross domestic product.[21] Like chronic disease prevalence, chronic disease costs also vary greatly between states.
Direct Costs
The health care costs of individuals with chronic disease tend to dwarf those of individuals without a chronic disease. Annually, direct health care costs for a patient with chronic disease average $6,032, approximately 5 times that of a person without a chronic disease.[22] These costs are primarily derived from more frequent hospitalizations and emergency room visits and greater prescription drug use.
The Milken Institute estimates costs associated directly with chronic disease totaled $1.1 trillion in 2016, with cardiovascular conditions accounting for 26.7 percent of costs, followed by diabetes with 17.2 percent of costs, Alzheimer’s accounting for 16.9 percent, and Arthritis and back pain accounting for 16.5 percent of costs.[23] Obesity—the greatest single risk factor for chronic disease—is responsible for nearly 44 percent of direct health care costs.[24]
Hospitalizations
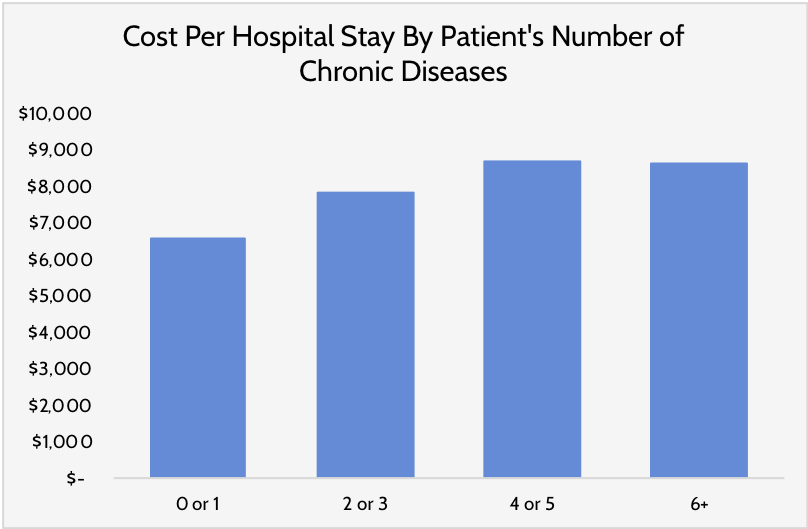
More frequent and longer lengths of stay are the drivers of higher hospitalization costs for individuals with chronic disease.[25] While only 3 percent of individuals with no chronic disease had an inpatient hospital stay in 2014, 10 percent of those with 3-4 chronic conditions and 24 percent of those with 5 or more did.[26] The length of one’s hospital stay is similarly impacted by the existence of chronic disease. Compared to those with 0 or 1 chronic condition, acute condition stays are 11 percent longer for those with 2 or 3 chronic conditions, 21 percent longer when 4 or 5 conditions are present, and 27 percent longer when 6 or more conditions are present.[27] The same pattern applies to stays associated with a chronic disease itself, as well as associated costs. For example, relative to patients with 0 or 1 conditions, costs per stay for ambulatory-care-sensitive conditions (those for which effective outpatient care can reduce the likelihood of hospitalization) were 19 percent higher for those with 2 or 3 chronic conditions, 32 percent higher for those with 4 or 5, and 31 percent higher for those with 6 or more, as shown in Figure 5.[28]
Figure 5:
Prescriptions
Individuals with chronic disease have greater prescription drug costs.[29] This higher cost is mostly due to the sheer number of prescriptions taken: In 2014, people with no chronic conditions took an average of 1 prescription per year while people with 3-4 chronic conditions took 24 and those with 5 or more conditions used 51 or more.[30] The high costs associated with the higher number of prescriptions can lead to non-adherence among patients as a strategy for reducing costs which often ultimately worsens health outcomes and increases the potential for an expensive hospitalization.[31] In fact, the Congressional Budget Office recently noted that for each dollar of improved medication adherence, medical costs are reduced by $2.00.[32] Poor medication adherence is particularly prevalent among seniors given that they are more likely to suffer from chronic disease, have multiple prescriptions, and have lower incomes. A number of experts argue that the standard practice of treating each chronic condition individually leads to over-prescription and sometimes harmful interaction, and as a result changing treatment practices could result in lower costs, better adherence, and fewer complications.[33]
Emergency Room Visits
Nearly 60 percent of all emergency room visits are associated with people with chronic conditions, at a cost of $8.3 billion in 2017.[34] It’s estimated that nearly 30 percent of such visits could be prevented or treated in a lower-cost setting if better managed.[35] The financial toll of these preventable visits is estimated at $2.5 billion.[36] People with chronic diseases inappropriately use the emergency room for a number of reasons. People often lack the knowledge needed to manage their disease, use their medications improperly, are unable to engage in effective self-care, fail to adhere to their treatment plan, or lack access to other forms of medical care.[37] For example, diabetes patients without health insurance have 168 percent more emergency department visits than their insured counterparts.[38] At the root of such overuse is a lack of understanding and appreciation for the importance of using alterative care settings, insufficient income necessary to keep oneself healthy, and, at times, mental health challenges.
Indirect Costs
Chronic disease creates costs far beyond medical care. Individuals with chronic disease can see their lives impacted in ways that are difficult to measure objectively but are potentially devastating nonetheless. Chronic disease affects people’s education, their livelihoods, and even social interaction. These consequences impact the overall welfare of those with a disease and their families, as well as society at large. In fact, the indirect costs of some diseases far outweigh the direct costs: the indirect cost of hypertension is estimated at 14.7 times the direct cost; prostate cancer, 6.8 times; chronic back pain, 5.7; osteoarthritis, 2.5; Type 2 Diabetes, 1.8.[39] One study estimates that the total cost of chronic conditions, after accounting for indirect costs, will total $42 trillion between 2016 and 2030, nearly 40 percent of which will be the result of lost employee productivity, as discussed below.[40]
Education and Human Capital
Chronic disease can interfere with the educational attainment of those who have a disease and their families. The spending required to treat a chronic disease has the potential to crowd out investing in higher education, a key determinant for future earnings.[41] Since low-income families often face a higher chronic disease burden, the increased costs associated with chronic disease make it even more difficult for children in these families to achieve upward economic mobility and thus, low-income families face a higher possibility of becoming entrenched in poverty. Chronic diseases such as addiction can affect a child’s future before they’re born. For example, smoking during pregnancy has been shown to impair a child’s cognitive and behavioral development and correlates with reduced human capital formation and productivity later in life.[42] People with a chronic disease are also more at risk for a premature death, an event that can severely impact their children’s educational attainment. Studies have shown that a child whose parent has recently died is twice as likely to drop out of school than children whose parents are still alive.[43]
Children also suffer educationally when they themselves have a chronic disease. Overweight or obese children struggle more in school than their peers due to the effects of their disease. They are often more likely to miss school, exhibit low self-esteem, and feel more shame.[44] These experiences are all significant obstacles to learning. Beyond learning, the essential social skills directly and indirectly taught in schools are highly valuable later in life. Chronic diseases that require careful monitoring, such as diabetes, can reduce children’s ability to fully participate at school and leave them feeling isolated in non-classroom settings such as recess and lunch.
Economic Well-Being
Having a chronic disease can often prevent people from having the financial resources they need to thrive. Due to chronic disease, individuals may lose the ability to perform their job duties to the extent that is expected. This effect is felt especially by people in low-paying jobs, which often require physical labor and allow for few, if any, days of leave.[45] Absences from work caused by chronic disease can result in reduced income or complete job loss.[46] Since the burden of care for those with chronic disease can often fall on relatives, their own productivity and income may fall as well.[47] Additionally, because of the aforementioned challenges for people with chronic diseases in getting an advanced education, such individuals may be less likely to get a high-paying job.
In more severe cases, chronic disease can prevent people from entering the labor force in the first place. One study conducted in Australia using data from the Australian National Health Survey found that labor force participation dropped by 3.9 percent for diabetic young men (aged 18-49) and 11.4 percent for diabetic older men (aged 50-64) when compared to their counterparts with no chronic disease.[48] This effect became more pronounced as subjects aged and suffered from more chronic diseases. For example, older men with four chronic diseases were employed at a rate of just 27.8 percent, whereas those without a chronic disease participated at a rate of 81.3 percent.[49]
The impacts of these consequences are significant and reach far beyond the individuals living with the disease: Labor productivity and labor force participation are the two key determinants of a country’s economic output.[50] Low productivity is associated with falling wages.[51] Low labor force participation rates are associated with slower economic growth, a higher dependency ratio, and higher tax rates.[52]
Social Well-Being
The disabilities associated with and the monitoring required for chronic diseases can be socially debilitating for many. Mental and physical chronic conditions can lead to harmful degrees of social isolation. Mobility restrictions and mental difficulties can make interacting with others difficult. Social isolation has been shown to have devastating effects on physical and mental health, as well, perpetuating a cycle of isolation and declining health.[53] When considering the vulnerabilities of people with chronic disease, the indirect effects of social isolation are important to understand. It has been shown that those who report frequent feelings of loneliness or who lack social connections suffer higher rates of morbidity and mortality, infection, depression, and cognitive decline.[54] Someone who is chronically ill and socially isolated may be less likely to adhere to their treatment regimen and, as a result, become more ill.
Conclusion
Chronic disease and its associated costs continue to climb in the United States, across all age groups. Given that the increased prevalence is not limited to elderly Americans, the burden of chronic disease will plague this country for many decades to come. Higher medical costs and a lower capacity to participate in the labor force or earn a livable wage as a result of chronic disease may worsen a person’s quality of life and, often, that of their family members, resulting in significant indirect costs. These effects persist and often worsen over time. The costs associated with chronic disease also place significant financial burdens on public resources and hinder economic growth. As the number of individuals with chronic disease grows, this burden will grow as well. Low-income individuals are more likely to suffer from chronic disease and may be disproportionately burdened by the costs and associated social and economic consequences. Interventions to prevent and better manage existing chronic disease can reduce direct costs and prevent many indirect costs from ever emerging, thus improving the economic well-being of individuals and the country as a whole.
[1] https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html
[2] https://www.cdc.gov/chronicdisease/about/index.htm#:~:text=Chronic%20diseases%20are%20defined%20broadly,disability%20in%20the%20United%20States.
[3] https://www.rand.org/blog/rand-review/2017/07/chronic-conditions-in-america-price-and-prevalence.html
[4] https://www.rand.org/blog/rand-review/2017/07/chronic-conditions-in-america-price-and-prevalence.html
[5] https://www.cdc.gov/pcd/issues/2015/14_0397.htm#:~:text=Approximately%2027%25%20of%20children%20in,this%20population%20have%20been%20limited.
[6] http://www.fightchronicdisease.org/sites/default/files/TL221_final.pdf
[7] https://www.cswe.org/getattachment/Centers-Initiatives/Gero-Ed-Center/Initiatives/Past-Programs/MAC-Project/Resource-Reviews/Health/CI-Sec1-Demographics.pdf.aspx#:~:text=At%20least%2080%25%20of%20people,illnesses%20(CDC%2C%202003).
[8] https://www.fightchronicdisease.org/sites/default/files/docs/GrowingCrisisofChronicDiseaseintheUSfactsheet_81009.pdf
[9] https://www.rwjf.org/en/library/research/2010/01/chronic-care.html
[10] https://www.rwjf.org/en/library/research/2010/01/chronic-care.html
[11] https://milkeninstitute.org/sites/default/files/reports-pdf/ChronicDiseases-HighRes-FINAL.pdf
[12] The remaining diseases not included in the figure showed a constant prevalence over the years.
[13] The unlabeled lines at the bottom represent the remaining diseases that follow the trend.
[14] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6351821/
[15] https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2014.0832
[16] https://www.healthaffairs.org/doi/full/10.1377/hlthaff.2014.0832
[17] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6887808/
[18] https://www.focusforhealth.org/chronic-illnesses-and-the-state-of-our-childrens-health/
[19] http://www.med.umich.edu/yourchild/topics/chronic.htm
[20] The percentages are the percentage of Medicare beneficiaries in the state suffering from a chronic disease. So, 14 percent diabetes in Colorado means that 14 percent of the Medicare beneficiaries in Colorado have been diagnosed with diabetes. The average disease score for each state was determined by averaging all the percentages for each disease within that state. For example, if only three diseases were being measured, and in Florida 2 percent of beneficiaries suffered from alcoholism, 20 percent from diabetes, and 15 percent from Alzheimer’s, the disease score for the state would be (2 percent + 20 percent + 15 percent )/ 3 = 12.3 percent.
[21] https://milkeninstitute.org/sites/default/files/reports-pdf/ChronicDiseases-HighRes-FINAL.pdf
[22] https://cdn.ymaws.com/www.chronicdisease.org/resource/resmgr/white_papers/cd_white_paper_hoffman.pdf
[23] https://milkeninstitute.org/sites/default/files/reports-pdf/ChronicDiseases-HighRes-FINAL.pdf
[24] https://milkeninstitute.org/sites/default/files/reports-pdf/ChronicDiseases-HighRes-FINAL.pdf
[25] https://www.hcup-us.ahrq.gov/reports/statbriefs/sb183-Hospitalizations-Multiple-Chronic-Conditions-Projections-2014.pdf
[26] http://www.fightchronicdisease.org/sites/default/files/TL221_final.pdf
[27] https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-016-1304-y
[28] https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-016-1304-y
[29] https://gh.bmj.com/content/bmjgh/3/1/e000505.full.pdf
[30] http://www.fightchronicdisease.org/sites/default/files/TL221_final.pdf
[31] https://gh.bmj.com/content/bmjgh/3/1/e000505.full.pdf
[32] https://www.cbo.gov/system/files/2019-05/55151-SupplementalMaterial.pdf
[33] https://gh.bmj.com/content/bmjgh/3/1/e000505.full.pdf
[34] https://healthitanalytics.com/news/chronic-conditions-account-for-8.3b-in-avoidable-ed-visits
[35] http://offers.premierinc.com/rs/381-NBB-525/images/Improving Care for Chronic Conditions, Premier.pdf
[36] http://offers.premierinc.com/rs/381-NBB-525/images/Improving Care for Chronic Conditions, Premier.pdf
[37] http://offers.premierinc.com/rs/381-NBB-525/images/Improving Care for Chronic Conditions, Premier.pdf
[38] http://offers.premierinc.com/rs/381-NBB-525/images/Improving Care for Chronic Conditions, Premier.pdf
[39] https://milkeninstitute.org/sites/default/files/reports-pdf/ChronicDiseases-HighRes-FINAL.pdf
[40] https://www.fightchronicdisease.org/sites/default/files/pfcd_blocks/PFCD_US.FactSheet_FINAL1%20(2).pdf
[41] https://www.who.int/management/programme/ncd/Chronic-disease-an-economic-perspective.pdf?ua=1
[42] https://www.who.int/management/programme/ncd/Chronic-disease-an-economic-perspective.pdf?ua=1
[43] https://www.who.int/management/programme/ncd/Chronic-disease-an-economic-perspective.pdf?ua=1
[44] https://www.who.int/management/programme/ncd/Chronic-disease-an-economic-perspective.pdf?ua=1
[45] https://www.americanactionforum.org/research/the-outsized-impact-of-the-coronavirus-pandemic-on-minority-communities/
[46] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4493930/
[47] https://www.who.int/chp/chronic_disease_report/part2_ch2/en/index7.html
[48] https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.175.5777&rep=rep1&type=pdf
[49] https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.175.5777&rep=rep1&type=pdf
[50] https://www.spglobal.com/en/research-insights/articles/declining-labor-force-participation-will-weigh-on-us-gdp-growth-and-fed-monetary-policy
[51] https://opentextbc.ca/principlesofeconomics2eopenstax/chapter/labor-productivity-and-economic-growth/
[52] https://www.bls.gov/opub/mlr/2018/beyond-bls/down-and-down-we-go-the-falling-us-labor-force-participation-rate.htm