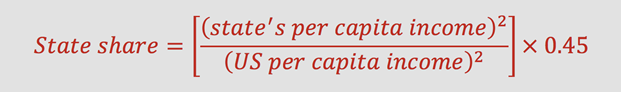Research
July 17, 2017
Primer: The Children’s Health Insurance Program (CHIP)
Background
The Children’s Health Insurance Program (CHIP) was established as part of the Balanced Budget Act of 1997 (BBA). The program was created to address coverage gaps between the poorest populations where children were covered by Medicaid, and the more affluent populations where families could afford private health care insurance.
In Fiscal Year (FY) 2015, CHIP covered 8.4 million children and cost the federal government $9 billion. In FY 2016, CHIP costs increased to $14 billion, and are projected by the Congressional Budget Office (CBO) to increase to $15 billion in FY 2017.[1] Comparatively, the total state share of CHIP funding was $4 billion in FY 2015, but is expected to fall to roughly $1 billion in FY 2017, as the federal government finances a much larger share of the program due to legislative changes which have recently gone into effect.[2]
Program Structure
The CHIP program itself is structured as a federal-state partnership. States may choose how to set up their own CHIP programs, whether as an extension of Medicaid, as a CHIP-Medicaid partnership, or as an independent, separately branded program. As of 2015, eight states and the District of Columbia. chose to use CHIP funds to expand Medicaid coverage to higher-income children while the remaining 42 states used a separate or combination program.[3] To a large extent, states may also determine their own eligibility levels, and incorporate cost sharing requirements into their programs.
Financing
Congress must authorize and appropriate an annual allotment of funds to be distributed to the states to finance the CHIP program, though CHIP funding is considered mandatory spending and funding is usually provided for multiple years at a time. Yet unlike Medicaid, which is an open-ended entitlement, total funding for CHIP is capped.
Each state is allotted a share of the total federal appropriation for that year based on the state’s historical program expenditures, growth in its child population, growth in national health care costs, and its Federal Medical Assistance Percentage (FMAP).[4] The FMAP is used to determine the federal funding match rate for the state Medicaid program, so in order to encourage states to create or expand children’s coverage, the traditional CHIP match rate (known as the enhanced FMAP or E-FMAP) is the state’s Medicaid FMAP plus about 15 percent, not to exceed 85 percent.[5] (This was temporarily changed by the Affordable Care Act (ACA), as discussed below). The original Medicaid FMAP is between 50 and 83 percent, and is determined by a statutory formula based on income:[6]
The traditional average CHIP match rate was 71 percent, meaning states must, on average, cover 29 percent of costs in order to receive their federal allotment; due to the aforementioned changes in the ACA, the current average match rate is 94 percent.[7]
States may typically rollover any unspent funds from one year to the next, though Congress occasionally rescinds at least of portion of unspent funds. Should a state face a shortfall even after receiving all available base CHIP funds, shortfall funding is available in the form of Child Enrollment Contingency Funds (available when a state’s CHIP enrollment exceeded target levels), Redistribution Funds (made available when after two years, unused state CHIP allotments are redistributed to states with shortfalls), and recently, if the others are insufficient, Medicaid match rates for expansion populations under the ACA. In the last several years, federal appropriations for CHIP have significantly exceeded actual expenditures; only twice has a state faced funding shortfalls and required use of contingency funds.[8]
Eligibility
CHIP covers families with income levels between 138 percent and 405 percent of the federal poverty level (FPL), depending on the state.[9] Thirty states’ eligibility levels are capped between 200 percent and 300 percent FPL and 19 states’ eligibility levels are higher than 300 percent FPL; although, states with caps above 300 percent FPL lose their E-FMAP and only receive the regular Medicaid FMAP for CHIP enrollees above 300 percent FPL.[10] More than 97 percent of CHIP enrollees have family income of 250 percent FPL or less.[11]
Infants born to Medicaid eligible women, some children in foster care or adoption programs, and some children with disabilities may also be eligible for CHIP regardless of income. Benefit packages vary by state, but are usually robust and all must include Early, Periodic Screening, Diagnosis, and Treatment (EPSDT) or a similar standard of care prescribed by the federal government.[12]
Provider Payments
Health care providers are reimbursed by the state either directly through fee-for-service (FFS), or through a managed care organization (MCO) contracted by the state to manage the cost and care of Medicaid and CHIP populations. Under FFS, the amount the provider receives for a given service is determined by a fee schedule created by each state that must meet minimum federal standards. This rate may be based on the costs of providing the service, a review of commercial payers’ reimbursement rates, or a percentage of what Medicare pays for equivalent services.[13]
Beneficiary Cost-Sharing
CMS imposes maximum nominal out of pocket costs for services paid for by Medicaid and CHIP.[14] States with Medicaid-extension CHIP must follow the cost-sharing rules of Medicaid: states can charge premiums to families with income levels over 150 percent FPL. States with separate CHIP programs may charge premiums and implement cost sharing. In both Medicaid-extension and separate CHIP programs, these costs cannot exceed 5 percent of a family’s income. Four states charge premiums for children on Medicaid, twenty-two states charge premiums on separate CHIP, and four states have CHIP enrollment fees.[15] CHIP children who are not covered under a mandatory eligibility group (for example, those over 300 percent FPL) may be given alternative out of pocket maximums. Children’s preventive care, hospice care, emergency services, family planning services, and pregnancy-related services are all also exempt from out of pocket costs.[16]
Subsequent Legislation
The original BBA only provided funding for CHIP through 2007. When the issue of reauthorization came before Congress, negotiations stalled and CHIP funding was simply extended without change until 2009.
CHIPRA
In 2008, CHIP again came up for debate in Congress, and funding was continued with the passage of the Children’s Health Insurance Program Reauthorization Act (CHIPRA) of 2009.[17] The legislation broadened eligibility for lawfully residing children and pregnant women, and addressed funding shortfalls. CHIPRA provided bonuses[18] in FY2009 through FY 2013 for states that increased their Medicaid (not CHIP) enrollment among low income children. Bonus eligibility also required implementation of four outreach and enrollment activities such as 12 months of continuous Medicaid and CHIP eligibility, elimination of Medicaid and CHIP asset testing, elimination of in-person interview requirements, use of joint Medicaid and CHIP applications, implementation of options to ease enrollees’ renewal processes, or implementation of an “express lane eligibility” (ELE) – where documentation from other social programs can automatically qualify a child for CHIP benefits.
The Affordable Care Act
In 2010, Congress passed the Affordable Care Act (ACA), extending CHIP funding through 2015. The law also provided for a 23-percentage point increase to states’ E-FMAP from 2016 through FY2019 – increasing the average CHIP E-FMAP to 94 percent in 2017, and shifting the range of federal financing upwards to 88 percent to 100 percent.[19]
Though funding was only appropriated through 2015, the ACA contains a Maintenance of Effort (MOE) clause that requires states to continue offering Medicaid and CHIP at current (2010) eligibility levels until 2019.[20] Although, there is a caveat to this that will result in different effects in each state, depending on the structure of their program should federal funding not be extended in future years. In states where CHIP is a Medicaid expansion program, without renewed funding, CHIP-eligible children will continue to be enrolled in the Medicaid program at the lower Medicaid federal match rate and at a higher cost to the states. States with independent CHIP programs, on the other hand, are not required to continue offering CHIP coverage once they have exhausted federal funds for the program.[21] To cope with a loss of CHIP funds, these states have the option of rolling CHIP-eligible children into Qualified Health Plans in the exchanges, imposing waiting lists or enrollment caps, or creating Medicaid screening procedures to ensure Medicaid-eligible children are enrolled in Medicaid and not CHIP. Of the 8.4 million children currently enrolled in CHIP, 4.7 million are in Medicaid-extension programs and 3.7 million are in separate CHIP programs; an estimated 1.1 million would likely become uninsured if the states quit offering coverage.[22]
Originally, CHIP was designed to target the children of families who could not afford to purchase family health insurance coverage. However, many children with CHIP health insurance should be able to participate in the ACA exchanges since they would also qualify for ACA subsidies. The American Action Forum (AAF) estimated in 2014 that 5.1 million children enrolled in or eligible to enroll in CHIP could obtain affordable health insurance through the exchange.[23] Unfortunately, coverage options within the ACA have proved to be an insufficient replacement for CHIP, as many children end up without coverage due to a loophole created by the Obama Administration’s implementation of the ACA. As long as an employer offers ‘affordable insurance’ to their employee, they have satisfied the employer mandate and there is no requirement to offer affordable coverage or any coverage to the individual’s family.[24] Because, in this scenario, a family member has been offered ‘affordable’ employer-sponsored insurance, albeit unaffordable for the family, the entire family becomes ineligible for ACA exchange subsidies. AAF estimated in 2014 that this loophole could affect as many as 2.28 million CHIP eligible children – 1.6 million who are currently enrolled in CHIP, and another 645,000 who are not enrolled but are eligible. In the absence of affordable coverage options on the exchange, CHIP provides these families with a way to obtain coverage for their children and avoid the individual mandate penalty. However, if CHIP funding is not extended, these children will lose this coverage option. The impact of the ACA’s family glitch will need to be considered during upcoming funding conversations.
MACRA
In April 2015, President Obama signed into law the Medicare Access and CHIP Reauthorization Act (MACRA) of 2015 with bipartisan support. Under the ACA, CHIP funding was set to expire in September 2015, making a new funding bill necessary for CHIP to continue. MACRA extended funding for the program through September 2017 with relatively few alterations to the program. Provisions in MACRA included: CHIP funding for FY2016 and FY2017, continuation of the 23 percent increase to the E-FMAP that was mandated in the ACA, extension of the “qualifying states” option through 2017, extension of the Child Enrollment Contingency Fund created in CHIPRA, increased investments in outreach and enrollment efforts for CHIP of $40 million, extension of express lane eligibility through FY2017, and extension of CHIPRA Child Health Quality Provisions.[25]
Now, Congress needs to appropriate additional CHIP funding before current funding expires on October 1, 2017. CHIP is viewed as a “must-pass” bill, but with the possible repeal of the ACA and modifications to Medicaid, the extension of CHIP funding has become more complicated. If Congress were to decline to appropriate funds for 2017-2019, states with Medicaid-extension CHIP would be required to support CHIP with state funds and states with separate CHIP programs would no longer have to provide insurance for CHIP children. Forcing states to carry that burden, of course, is politically infeasible. How to proceed with CHIP funding must be discussed along with other possible policy changes, such as a repeal of the MOE, or broader retooling of the CHIP program.
CHIP Under Trump’s Budget Proposal
The Trump Administration’s first budget proposes extending CHIP funds through 2019 and eliminating the 23 percent increase to the E-FMAP that strains the federal government’s budget. President Trump also proposed eliminating the MOE so states have the ability to make the necessary modifications to make their own CHIP programs economically feasible. They also plan to allow children ages 6-18 with family income levels 100 percent to 133 percent of FPL (known as stair-step children) who were switched from CHIP to Medicaid under the ACA to return to CHIP. According to the CBO, these provisions would save $5.8 billion over the next 10 years.[26] Under the proposed budget, about half of states would lose federal matching funds for children in families with income up to 250 percent FPL as a result of an eligibility cap on federal matching funds, which would likely lead to reduced eligibility for children.
This Primer serves as an update to earlier editions of this paper written by Brittany La Couture & Angela (Boothe) Wiles.
[1] https://www.cbo.gov/system/files/115th-congress-2017-2018/reports/52801-june2017outlook.pdf
[2] Medicaid and CHIP Payment and Access Commission (U.S.), March 2017, Report to the Congress on Medicaid and CHIP, Washington, DC: MACPAC, Medicaid and CHIP Payment and Access Commission, https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf.
[3] https://ccf.georgetown.edu/2017/02/06/about-chip/
[4] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[5] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[6] Section 1101(a)(8)(B) & Section 1905(b) of the Social Security Act
[7] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[8] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[9] https://www.benefits.gov/benefits/benefit-details/607
[10] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[11] https://www.macpac.gov/wp-content/uploads/2017/03/March-2017-Report-to-Congress-on-Medicaid-and-CHIP.pdf
[12] http://www.kff.org/report-section/medicaid-and-chip-eligibility-enrollment-renewal-and-cost-sharing-policies-as-of-january-2017-premiums-and-cost-sharing/
[13] CMS, Financing and Reimbursement, http://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Financing-and-Reimbursement/Financing-and-Reimbursement.html.
[14] https://www.medicaid.gov/medicaid/cost-sharing/out-of-pocket-costs/index.html
[15] http://www.kff.org/report-section/medicaid-and-chip-eligibility-enrollment-renewal-and-cost-sharing-policies-as-of-january-2017-premiums-and-cost-sharing/
[16] CMS, Out-of-Pocket Cost Exemptions, http://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Cost-Sharing/Cost-Sharing-Exemptions.html.
[17] CRS, H.R. 2: The Children’s Health Insurance Program Reauthorization Act of 2009, Jan. 14, 2009, http://assets.opencrs.com/rpts/R40130_20090114.pdf.
[18] Bonus payments equal 15 percent of a state’s share of the enrollee’s projected per capita Medicaid expenditures for enrollees that represent growth below 10 percent of baseline; payment is 62.5 percent of state’s share of Medicaid expenditures for enrollees above 10 percent growth over baseline.
[19] CRS, State Children’s Health Insurance Program: an overview, Jul. 3, 2014.
[20] CRS, State Children’s Health Insurance Program: an overview, Jul. 3, 2014.
[21] https://www.macpac.gov/wp-content/uploads/2017/03/Federal-CHIP-Funding-When-Will-States-Exhaust-Allotments.pdf
[22] https://www.macpac.gov/wp-content/uploads/2017/03/Federal-CHIP-Funding-When-Will-States-Exhaust-Allotments.pdf
[23] Conor Ryan, Who Still Needs CHIP?, Sept. 15, 2014, https://www.americanactionforum.org/weekly-checkup/who-still-needs-chip.
[24] Angela Boothe & Christopher Holt, CHIP Extension and How the ACA Fails Families, AAF Insights, Jun. 24, 2014, https://www.americanactionforum.org/insights/chip-extension-and-how-the-aca-fails-families.
[25] CRS, “Federal Financing for the State Children’s Health Insurance Program (CHIP), https://fas.org/sgp/crs/misc/R43949.pdf.
[26] http://www.kff.org/medicaid/fact-sheet/presidents-2018-budget-proposal-reduces-federal-funding-for-coverage-of-children-in-medicaid-and-chip/