Weekly Checkup
March 29, 2019
Observations From a Wild Week in Health Care
It’s been a wild week for those who follow health care policy. First, the Trump Administration decided to change its position on the ongoing Affordable Care Act (ACA) litigation working its way toward the Supreme Court and argue for the entire law to be thrown out as unconstitutional. Second, a federal judge ruled against the administration’s pursuit of work requirements in the Medicaid program via state waivers. Finally, yet another federal judge overturned the administration’s rulemaking on association health plans (AHPs). While the path forward on all fronts is murky, here are a few observations.
President Trump’s decision to change the stakes in the legal battle over the ACA and health care policy is somewhat of a non-event. The Department of Justice’s change in posture toward the Texas v. Azar lawsuit is one of degree that is unlikely to have a decisive impact on the ultimate resolution of the case. It does, however, create real problems for Congress. As detailed in a previous Weekly Checkup, the divided 116th Congress is hardly in a position to enact comprehensive health legislation. If the Supreme Court were to strike down the law in its entirety, it is almost impossible to imagine House Democrats, Senate Republicans, and the White House being able to coalesce around a comprehensive alternative.
The easiest course of action would have been for congressional Republicans and Democrats to unite and repeal the individual mandate, in effect ending the basis for the lawsuit and preserving the status quo for the moment. But with the White House action motivated at least in part by a desire to pressure congressional Republicans to rejoin the health care fight—and one supposes avenge one of the president’s more glaring legislative losses—that course of action may no longer be politically viable for Republicans. Instead, both sides may be left to hope the courts bail them out.
Moving to Medicaid—and setting aside the particulars of the Arkansas and Kentucky Medicaid waivers that were struck down—the conflict arises because of the philosophical differences between conservatives and liberals when it comes to Medicaid. Fundamentally, most conservatives look at Medicaid as part of a safety net that should be invoked when the best efforts of an individual still leave him poor and vulnerable. In contrast, most liberals look at Medicaid simply as another tool for expanding health coverage to as many people as possible. As a result, liberals don’t share the concern of many conservatives that Medicaid has ballooned to cover one-fifth of the U.S. population. Similarly, conservatives see work requirements as consistent with individuals doing all they can on their own before turning to a social safety net program, while liberals see them as an artificial impediment to their fundamental goal of increasing coverage.
Thursday’s decision against the administration’s AHP rule is disappointing, as expanding access to AHPs has long been a conservative policy objective. But while news coverage—and Judge Bate’s own rhetoric in the ruling—focus on the AHP rule as an underhanded attempt to circumvent the ACA, the ruling is really based on the definition of employers and employees under the Employee Retirement Income Security Act of 1974. The key line from the ruling says, “Because the final rule stretches the definitions of ‘employer’ beyond what the statute can bear, the final rule is unlawful.” While the underlying policy may be desirable, to the degree this ruling is legitimately checking regulatory overreach beyond what is allowed by statute it is a positive development.
Combined, all three events raise the stakes for the Texas v. Azar suit. For some time, the administration has been working to build an alternative health care system to Obamacare. Through waivers and rulemaking, the White House and federal agencies have worked to provide more, affordable options and to tackle entitlements—all things that seem beyond the capacity of Congress at the moment. As the White House runs into road blocks in these efforts, the outcome of the ACA lawsuit becomes more important.
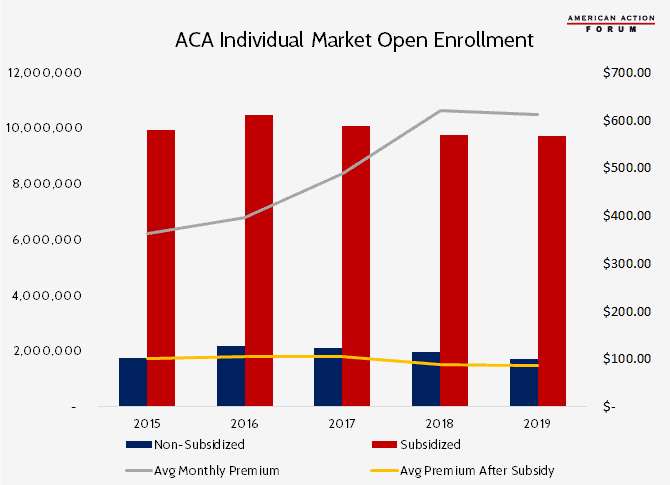
Chart Review
Tara O’Neill Hayes, Deputy Director of Health Care Policy
This week, the Centers for Medicare and Medicaid Services released enrollment data for this year’s individual market open-enrollment period. There was much speculation that enrollment would significantly decline because of the various changes that have been made to the Affordable Care Act since President Trump took office, namely eliminating the individual mandate and allowing for expanded use of short-term insurance plans and association health plans. The latest figures show only slight decreases in enrollment: overall: Roughly 300,000 fewer people enrolled, with 83 percent of that decline among non-subsidized individuals who are the most sensitive to high premium rates.
From Team Health
Assessing Efforts to Curb Inappropriate Use of the Emergency Room
Deputy Director of Health Care Policy Tara O’Neill Hayes examines how insurers and Medicaid are seeking, understandably, to reduce unnecessary emergency room use, and why these efforts could backfire. A better solution to the problem of rising health care costs linked to unnecessary ER use likely involves expanding access to alternative care settings, she writes.
Worth a Look
STAT News: As the FDA warns against ‘young blood,’ an ambitious Silicon Valley startup tests a cocktail for Alzheimer’s
Modern Healthcare: Insurers ask CMS for more flexibility on grandfathered ACA plans
New York Times: At 71, She’s Never Felt Pain or Anxiety. Now Scientists Know Why.