Weekly Checkup
June 12, 2020
Revisiting Infection Disparities
Recently, the Weekly Checkup reviewed data from a retrospective cohort study looking at racial disparities in COVID-19 hospitalization. The data pointed to differences in the presence of comorbidities but especially in the forms of insurance, and such factors may lend to the disproportionate impact of COVID-19 on Black patients. Recently, the Department of Health and Human Services (HHS) released an initiative to better understand the impact of COVID-19 on minority populations. This initiative includes new data collection and dissemination via the Centers for Disease Control and Prevention (CDC), including data on race and ethnicity. Given the new data and research on the subject along with recent efforts by states to reopen their economies, it is worth revisiting this topic and considering how various groups of people may be affected.
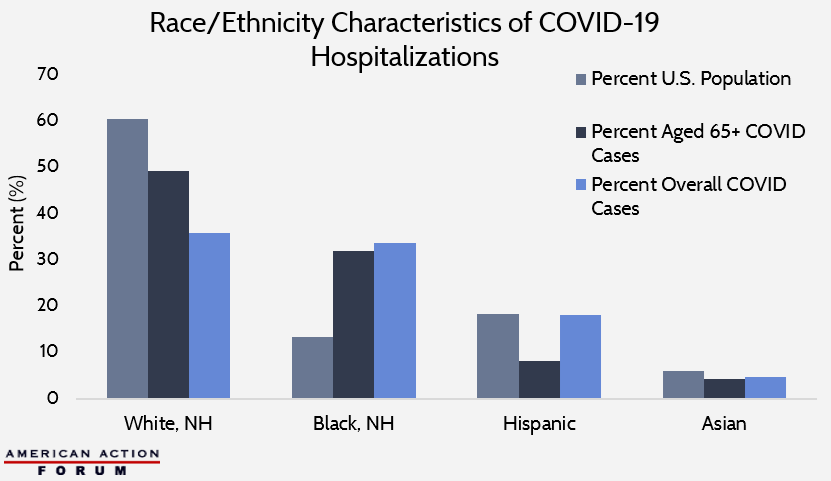
The chart below highlights some statistics taken from the CDC. White, non-Hispanic (NH) people make up 60.4 percent of the population and 35.7 percent of total COVID-19 hospitalizations. Black, NH people make up only 13.4 percent of the population but account for 33.6 percent of overall COVID-19 hospitalizations. Hispanic people account for both 18 percent of the population and of overall hospitalizations. Asian people are 5.9 percent of the population and account for 4.7 percent of hospitalizations, although the data for hospitalizations combine Asians and Pacific Islanders. COVID-19 hospitalizations for those 65 years of age and above follow similar trends apart from the Hispanic population, whose hospitalizations are skewed toward younger ages.
As discussed before, Black patients have a higher prevalence of comorbidities such as diabetes mellitus and hypertension, and these conditions are strongly suspected of contributing to COVID-19 severity. As the research highlighted a couple of weeks ago alludes to, however, the risk associated with comorbidities when analyzed across racial and ethnic lines may be confounded or mediated by other variables. This is where research from AAF’s Tara O’Neill Hayes is quite illuminating, as there are many factors likely contributing to the outcomes observed in addition to personal health, including jobs and living environment.
Baseline health status is important, but people of racial and ethnic minorities are also more likely to work in lower-paying sectors that increase their risk of exposure. A particularly important piece of data Hayes cites in this regard reports low-paying jobs in nursing homes and residential care services being more likely to be held by Black women, who account for about 23 percent of nursing care facility employees and 24 percent of employees for other residential care facilities. As I have mentioned previously, this fact alone is a monumental risk that cannot be overstated.
Tightly coupled with disparities in wages and particular job sectors is the fact that people belonging to minority groups are more likely to live in highly dense areas and be a part of multi-generational households. Since COVID-19 primarily transmits indoors, working in higher-risk sectors of the economy and living in higher-density housing increase the risk of infection.
As the country continues to move forward with reopening, where does this set of facts leave us? While it is probable that we will observe upticks in COVID-19 cases (as are already apparent in some places), we should focus on where exactly these cases are coming from. This mixture of variables suggests any uptick in cases may disproportionately come from minority communities already at a higher risk. Every level of government, from Congress to municipalities, should utilize these incoming data to tailor testing availability and resource distribution to areas most vulnerable to an increase in cases.
Worth a Look
Axios: More price-fixing lawsuits hit the generic drug industry
New York Times: Covid-19 Patient Gets Double Lung Transplant, Offering Hope for Others