Weekly Checkup
March 5, 2021
The Next Reconciliation Bill
This week the Senate took up the House-passed reconciliation package, otherwise known as the American Recovery Plan, with amendment votes slated to begin as early as today. Senate Democrats have made a few notable tweaks to the legislation’s health policy sections, but with passage largely a foregone conclusion, attention is already starting to turn to what comes next.
There have been a few changes since we last reviewed the reconciliation package’s health care provisions. For one thing, the COBRA subsidy—which doesn’t make much sense at this point in the pandemic—is being increased, from the 85 percent provided in the House-passed text, to 100 percent. This appears to have come at the behest of labor unions and will almost double the cost of the benefit, according to the Congressional Budget Office. The Senate is also adding an additional $8.5 billion to shore up rural hospitals. Those funds are in addition to the $175 billion already allocated for providers in past COVID-19 relief legislation, but also short of the $35 billion hospitals were seeking. Additionally, in what looks like a small, if temporary, win for the pharmaceutical industry, changes to Medicaid’s inflation penalties—which could result in drug makers being forced to pay state Medicaid plans when their drugs are used (instead of, you know, the normal arrangement where companies are paid FOR their products)—are pushed back a full year in the Senate draft. Otherwise, however, this is largely the package we’ve already reviewed, here, here, here, and here.
While there are still a few hurdles to traverse, many policy watchers are already putting this reconciliation effort in the rearview mirror and starting to speculate about what comes next for the Biden Administration’s health policy agenda. The conventional wisdom at this point is that any significant health policy effort by the Biden Administration will have to come via another reconciliation bill, executive action, or a combination of both. Setting aside what is sure to be a robust focus on executive action, what might Biden pursue legislatively?
Biden’s big goal is a public option insurance plan modeled on Medicare that would compete with private insurers on the Affordable Care Act’s (ACA) health insurance exchanges. That initiative is unlikely to fly under the rules of reconciliation. While some argue that an effort to lower the Medicare age could pass muster, there is past precedent that you can’t raise the Medicare age in reconciliation. In the end, the most promising policies for qualifying under reconciliation are those already included in the current reconciliation bill: increasing the generosity of the ACA’s subsidies and lifting the income eligibility cap. But those changes are temporary due to reconciliation restrictions on increasing the deficit outside of the 10-year budget window. President Biden will almost certainly want to extend those policies beyond the two years they would last under the current proposal. But making those changes permanent, even through reconciliation, would require offsetting the cost.
Fortunately for Biden, Democrats have a host of policies aimed at reducing the cost of prescription drugs—and punishing drug makers for turning a profit—waiting in the wings. Not every drug policy idea would work under reconciliation, but many could. And there is broad bipartisan support for at least one proposal to substantively restructure the Medicare Part D drug benefit, which could provide some savings depending on specifics.
Despite the relative ease with which Democrats are moving the current reconciliation bill, passing legislation through reconciliation is a delicate process, and it’s far from a forgone conclusion that another reconciliation bill will proceed as easily, or that the Biden Administration will choose to focus its limited reconciliation slots on health care. But if President Biden decides to go all in legislatively on health care, the most likely package would be one that makes the ACA changes permanent and pays for it through long-sought progressive drug policy reforms.
Podcast
AAF’s Christopher Holt dives into the current proposals surrounding the ACA as well as its trajectory as a law in the latest episode of The AAF Exchange.
Chart Review: COVID-19 Vaccine Administration by Country
Ashley Brooks, Health Policy Intern
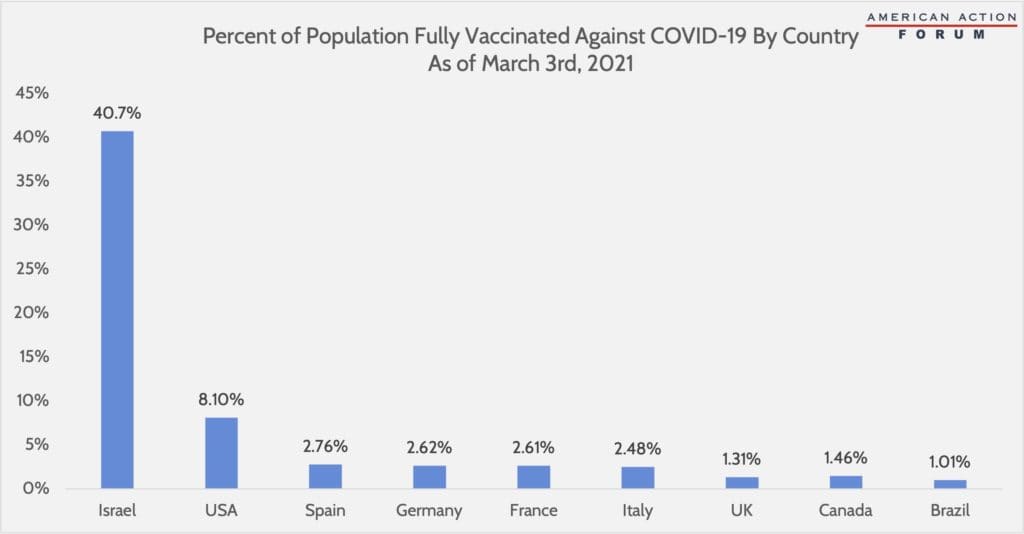
Last week, the Food and Drug Administration approved emergency use of the Johnson & Johnson single-dose COVID-19 vaccine, which is expected to drastically speed up the vaccination process. Additionally, this week the Biden Administration announced a deal between Merck and Johnson & Johnson to further expedite the production and distribution process. These developments make Biden’s promise of enough vaccine for every American adult by the end of May a more realistic proposition. The United States initially experienced numerous hurdles in the COVID-19 vaccine rollout, but it has some of the most aggressive vaccine-administration rates in comparison to other leading nations, as the chart below shows. As of March 3rd, Israel has the greatest proportion of its population fully vaccinated against COVID-19, having vaccinated just over 40 percent. While these rates are impressive, Israel’s total population equals just under 3 percent of the entire U.S. population, and its landmass equals that of New Jersey. Further, Israel stores over 5 million vaccines in a centralized facility, minimizing disruption during vaccine distribution to other regions within the nation. As shown in the chart below, many European nations have a slower administration rate, having fully vaccinated approximately 2.6 percent of their total populations thus far, as seen in Spain, Germany, France, and Italy, all displaying similar rates.
Sources: Our World in Data and World Population Review
Tracking COVID-19 Cases and Vaccinations
Ashley Brooks, Health Policy Intern
To track the progress in vaccinations, the Weekly Checkup will compile the most relevant statistics for the week, with the seven-day period ending on the Wednesday of each week.
| Week Ending: | New COVID-19 Cases: 7-day Average |
Newly Fully Vaccinated: 7-Day Average |
Daily Deaths: 7-Day Average |
|
March 3, 2021 |
62,555 |
635,268 |
1,921 |
|
Feb. 24, 2021 |
66,305 |
781,716 |
2,059 |
|
Feb. 17, 2021 |
76,723 |
693,786 |
2,687 |
|
Feb. 10, 2021 |
103,553 |
652,599 |
3,009 |
|
Feb. 3, 2021 |
134,248 |
444,164 |
3,013 |
|
Jan. 27, 2021 |
161,803 |
308,208 |
3,296 |
Sources: Centers for Disease Control and Prevention Trends in COVID-19 Cases and Deaths in the US, and Trends in COVID-19 Vaccinations in the US
Note: The U.S. population is 330,113,974.
Worth a Look
The Hill: US in talks with allies to counter China’s vaccine diplomacy
Axios: The cost of the pandemic is catching up to health insurers